Understanding the complexities of carbapenem-resistant pathogens
Introduction
Infection control is a critical aspect of healthcare, particularly with the growth of carbapenem-resistant pathogens. These pathogens can adversely impact patient care, prolonging hospital stays, and increasing healthcare costs. Treating these superbugs requires new solutions. This article explores understanding carbapenem-resistant pathogens and how Endurocide® Antimicrobial Plus Curtains can aid in infection prevention.
Pathogens are classed as carbapenem-resistant when specific organisms become resistant to the carbapenem family of antibiotics.
Understanding carbapenem-resistant pathogens is complex due to various strains and acronyms used to describe them. Different countries can use these acronyms interchangeably, which doesn’t take account of the complex differences in their meanings. Furthermore, there are geographical variances between carbapenem-resistant pathogen strains and their impact on Hospital Acquired Infections (HAIs).
- Acronyms – a break down
- Carbapenem-resistant pathogens within the Enterobacterales family
- Carbapenem Producing Organisms
- Terminology around the world
- How do you select an antimicrobial product?
- Why choose Endurocide® Antimicrobial Plus Curtains?
Acronyms – a break-down
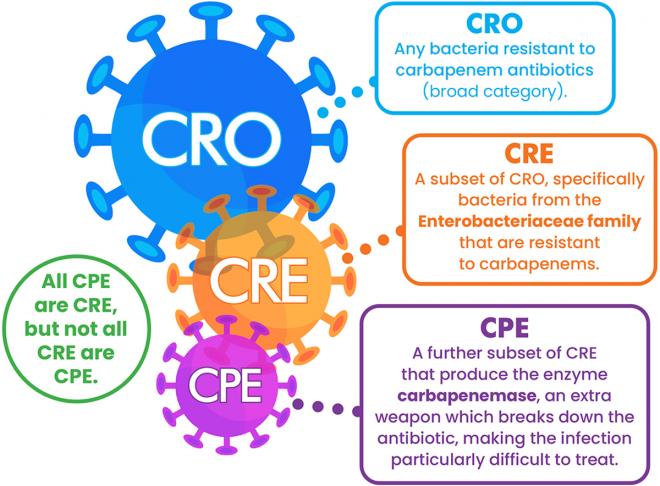
To better understand the nuances of carbapenem-resistant pathogens, let’s explore the acronyms commonly used to classify these organisms and their resistance mechanisms:
| Acronym | Meaning | Explanation |
CRO |
Carbapenem-Resistant Organisms | This is a general term used to describe any organisms that are resistant to the carbapenem family of antibiotics.This group of antibiotics are broad-spectrum and are often used against many Gram-positive and Gram-negative bacteria and are among some of the most successful drugs for treating infections caused by bacteria. Until recently they were often considered a ‘drug of last resort’.
However, the emergence and spread of antibiotic resistance to these drugs is a serious issue, which presents severe challenges for hospitals. |
CRE |
Carbapenem-Resistant Enterobacteriaceae | CRE specifically refers to bacteria in the Enterobacterales family that resist carbapenem antibiotics due to carbapenemase enzymes. These enzymes break down the antibiotics and prevent them from killing the bacteria. Pathogens harbouring these enzymes are sometimes referred to as “superbugs” because they are generally resistant to most/all other antibiotics and the treatment of infection is very challenging.Consider CRE as bacteria with a strong shield against powerful antibiotics.CRE are a subset of CRO. While CRO includes all bacteria resistant to carbapenems, CRE focuses specifically on carbapenem-resistant bacteria within the Enterobacterales family. As such all CRE can be classed as being part of the broader category of CRO, but not all CRO are CRE. |
CPO |
Carbapenemase-Producing Organisms | CPO refers to any bacteria that produce carbapenemase enzymes, which alter carbapenem antibiotics and render them ineffective against infections.
So, if carbapenem antibiotics are like a key that unlocks a door to kill the bacteria, the carbapenemase enzyme are like a lock that changes its shape so the key no longer fits. Whilst the CRE and CPE terminologies are focused solely on the Enterobacterales family of pathogens; the CPO acronym can be used to cover any organism that produces the carbapenemase enzyme. As such, CPO is a broad term that can include a variety of bacteria from different families, such as Pseudomonas aeruginosa, Acinetobacter species, as well as Enterobacterales. |
CPE |
Carbapenemase-Producing Enterobacterales | CPE Refers to pathogens within the Enterobacterales family capable of producing carbapenemase enzymes. It is a subset of both CRE and CPO categories:
|
Back to top
Carbapenem-resistant pathogens within the Enterobacterales family
In the Enterobacterales family, common bacteria that may become carbapenem-resistant include:
| Pathogen | Comments | CRE or CPE? |
| Escherichia coli
Found in the intestines, some strains cause severe infections if carbapenem-resistant. |
Some E. coli strains are CPE, producing carbapenemases like KPC, NDM, or OXA-48. | Can be either CRE or CPE, depending on the strain and the presence of carbapenemase enzymes or other mechanisms of resistance.
Would be considered CRE if the strain didn’t produce carbapenemase enzymes. |
| Klebsiella pneumoniae
Known for causing pneumonia, bloodstream infections, especially in healthcare settings. |
Klebsiella pneumoniae is a major cause of CPE, with strains often producing carbapenemases such as KPC, NDM, or OXA-48. | |
| Enterobacter species
These bacteria can cause various infections, including respiratory and urinary tract infections. |
Some strains can be CPE, particularly Enterobacter cloacae and Enterobacter aerogenes. | |
| Citrobacter species
These bacteria can lead to infections in the urinary tract, respiratory tract, and other areas. |
Some Citrobacter species can be CPE, especially Citrobacter freundii and Citrobacter koseri, known for producing carbapenemases. | |
| Proteus species
Can cause urinary tract infections and other types of infections. |
Proteus species are typically not known for producing carbapenemases, so are usually considered CRE rather than CPE. | Usually considered CRE |
| Serratia marcescens
Known for causing infections in the urinary tract, respiratory tract, and bloodstream, particularly in hospitalised patients. |
Generally, Serratia marcescens is not commonly associated with carbapenemase production, so are usually considered CRE rather than CPE. | Usually considered CRE |
Back to top
Carbapenem Producing Organisms
Pathogens grouped as CPOs due to their potential for carbapenem resistance caused by producing the carbapenemase enzyme, include:
| Pathogen | Family | Comments |
| Any CPE pathogens listed above | CPE
(Enterobacterales family) |
CPE pathogens often include: E.coli, Klebsiella pneumoniae and Enterobacter species known to produce carbapenemases. |
| Pseudomonas aeruginosa
Often found in hospitals, this bacteria can cause a range of infections, particularly in patients with weakened immune systems. |
Pseudomonadaceae Family
(Non-Enterobacterales) |
Pseudomonas aeruginosa often develops carbapenem resistance, referred to as CRPA when carbapenemases like VIM, IMP or NDM are present. |
| Acinetobacter baumannii
Commonly found in healthcare settings, it can cause infections in the blood, urinary tract, lungs, and wounds. |
Moraxellaceae Family
(Non-Enterobacterales) |
Acinetobacter baumannii often develops carbapenem resistance, referred to as CRAB when carbapenemases like OXA-23 or NDM are present. |
Back to top
Terminology around the world
| Pathogen | Comments |
| UK | In the UK, the terms CRE and CPE are often used interchangeably, but with a growing emphasis on the use of CPE. |
| Europe | As in the UK, European countries use both CRE and CPE, with a trend towards favouring CPE. |
| Australia | Australia predominantly uses the term CPE to highlight the specific mechanism of resistance. There is also use of the term CPO. |
| New Zealand | New Zealand predominantly uses the term CPE to emphasise the specific mechanism of resistance. |
| Canada | Canada uses both CRE and CPE, but leans towards CPE for specifying resistance. |
| India | In India, the terms CRE and CPE are often used interchangeably, but there is a growing recognition of the importance of distinguishing between them. |
| South Africa | South Africa uses both CRE and CPE terminology, with an increasing emphasis on CPE to accurately describe the resistance mechanism. |
| Brazil | In Brazil, the terms CRE and CPE are both used, with a trend towards specifying CPE in clinical and diagnostic contexts. CRE is used more broadly in public health discussions. |
| Singapore | In Singapore, there is a clear distinction between CRE and CPE, with CPE used specifically to indicate carbapenemase production. |
| Malaysia | In Malaysia, both CRE and CPE terminologies are used, with a preference towards specifying CPE to denote carbapenemase production. |
| China | In China, both CRE and CPE are both recognised terms, with a growing emphasis on distinguishing specific CPE. |
| Japan | In Japan, there is a clear distinction between CRE and CPE, with CPE used specifically to indicate carbapenemase production. |
Back to top
How do you select an antimicrobial product?
Understanding the complexities of carbapenem-resistant pathogens, particularly the variations in strains and terminology like CRE and CPE, is crucial.
Specific strains may vary by region or country, which complicates testing and product selection. However, it is impractical to test against every strain. Typically, laboratories use representative strains to assess antimicrobial effectiveness, as often there is minimal variation in antimicrobial resistance among different strains of the same organism.
Summary: When choosing antimicrobial products, consider their effectiveness against a range of relevant pathogens rather than every possible strain variation.
Back to top
Why choose Endurocide® Antimicrobial Plus Curtains?
It is essential to take a layered approach to the role of infection prevention and control in healthcare settings. As high-touch points within a healthcare setting, curtains play a crucial role in either aiding or hindering infection control practices. Benefits include:
- The dual mechanism of trapping and killing pathogens, which helps break the chain of infection.
- Effectiveness against bacteria, fungi, spores, enveloped viruses, and mycobacteria.
- Maintaining effectiveness over time, surpassing basic antimicrobial alternatives.
Endurocide® Curtains have been independently tested and proven to be effective against 29 different pathogens, including the following pathogens which are commonly thought of as being carbapenem-resistant:
- Acinetobacter baumannii
- Acinetobacter baumannii (CRAB)
- Acinetobacter baumannii (MDRA)
- Escherichia coli
- Extended Spectrum Beta-lactamase (ESBL) Escherichia coli
- Extended Spectrum Beta-lactamase (ESBL) Klebsiella pneumoniae
- Klebsiella pneumoniae
- Pseudomonas aeruginosa
Endurocide® Antimicrobial Plus Curtains have been tested and shown to be effective against specific carbapenem-resistant pathogens for up to two years after manufacture. They have also been tested in numerous independent, in-hospital peer-review trials, including:
| Country | Focus | Link |
| Hong Kong | Wide-scale hospital trial in Hong Kong, comparing Endurocide® Curtains against Silver and polyester curtains. | Click or tap here |
| Australia | Long -term hospital trial examining the performance of Endurocide® Curtains over 24-months. | Click or tap here |
| USA | Cost analysis trial examining the cost savings to be made by switching to Endurocide® Curtains. | Click or tap here |
Back to top
| If you would like to discuss your specific infection control needs and how Endurocide® Curtains can help, please contact us at: | |
Back to top




